Realizing the digital hospital through operational excellence
Hospitals in the U.S. are under pressure. Topline revenue growth (Figure 1) is falling as commercial reimbursement rates slow,1 combined with negligible increases in Medicare rates.2 Rising costs related to an aging population and a shift toward value-based care post the Affordable Care Act are further putting hospitals under immense financial pressure. The average operating margins for hospitals declined from 4.15% in 2015 to 2.56% in 2017, according to a Navigant report.3
Figure 1. US hospital revenue growth has declined in recent years
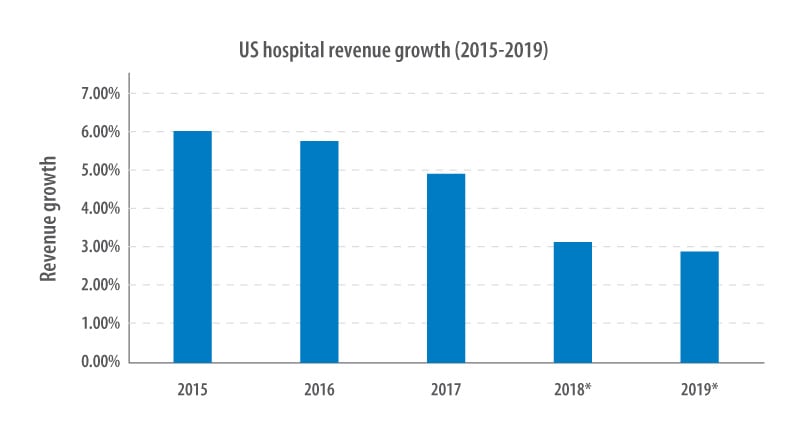
*2018 and 2019 figures are estimated.
Source: https://www.statista.com/forecasts/311200/hospitals-revenue-in-the-us
The competition further compounds these challenges. Technology companies like Apple, Amazon and Google, as well as a slew of startups, are launching digital health services that aim to bring transparency and remove the inefficiencies in the health care industry. Hospitals also face competition from outpatient facilities such as drugstore chain CVS, which has a network of health clinics that can be an alternative to many outpatient services.
To remain competitive, hospitals have to look beyond technology investments for patient treatment and embrace digital transformation for their daily operations and processes, removing inefficiencies like revenue leakage and long revenue cycles and improving cash flow and the customer experience.
Benefits of digital operational excellence
The return on investment for hospitals that have digitized their operations has been immediate. For example, in two and a half years, the Methodist Healthcare System of San Antonio was able to add more than $150 million to its profit line by optimizing its multihospital operations through the automation of its capacity management process.4
Figure 2 provides some recommendations on where hospitals can start on digital transformation for operations.
Some key areas where operational excellence can deliver financial results and improved experiences:
- Automated billing and claims systems can potentially result in a savings of $7 billion for the health care system. Several studies estimate the average cost of a manual transaction is $5, and it reduces to approximately $1.60 for an electronic transaction, which can potentially result in saving $7 billion annually by converting everyday transactions (e.g., claim submission, eligibility, benefit verification, prior authorization, claim status inquiry, claim payment and remittance advice) from manual to electronic.
- The supply chain is complex and the most difficult thing to change in health care; however, hospitals availing the services of group purchasing organizations are seeing significant benefits. A Healthcare Supply Chain Association report5 estimates that hospitals can achieve a cost savings of $392.2 billion and $864.4 billion between 2013 and 2022, respectively, using GPOs.
- Claims automation can minimize claim denials and increase revenue. An incorrect claim is costly in both time and money. Research data6 indicates that hospitals in the U.S. lose about $262 billion per year on denied claims and that, on average, it costs $118 to secure payment on a denied claim.
- Revenue cycle automation and optimization can ensure that the revenue cycles are operating at maximum efficiency. Revenue cycle inefficiencies cost about 15 cents of every health care dollar spent, per a McKinsey report (2009).7
- Automating routine and mundane tasks can also help in saving labor costs. Analysis of financial reports of hospitals indicates that labor costs contribute to 60% of operating expenses.
- Data for operational efficiency: Automation and robotic process automation can provide data that is critical for analytics and insights into how to provide better care for patients and to also maintain data privacy. This data can be used to predict demand and manage wait times and resources (bed capacity). Data, in combination with the internet of things(IoT), enables hospitals to create more products in preventive care and specialized disciplines while reducing costs and improving access through telemedicine. Effective use of existing resources also saves on further capital expenditure.
- From a qualitative perspective, the customer experience can also be significantly improved through enabling seamless admission procedures, reduced wait times or digitized food menus — all enabled by operationally efficient core services.
Figure 2. Digital transformation opportunities in hospital systems
| System | Operations and processes | Capabilities required for digital transformation | Benefits |
|---|---|---|---|
| Send routine appointment requests to a specific work queue based on defined criteria | RPA bots (trained to do a particular repetitive task): input information, retrieve information, display output, recognize known patterns | Improve customer experience | |
| Prior authorization | RPA | Reduce front-end revenue leakage | |
| Physician notes | RPA | Increase collections | |
| Eligibility checks | RPA | Improve cash flow | |
| Coordination of benefits | RPA | Improve cash flow | |
| Coordination of benefits | RPA | Improve cash flow | |
| Find other sources of funding | RPA | Improve cash flow | |
| Enhance patient communication | RPA | Improve customer experience | |
| Expedite cost-estimate generation | RPA | Improve cash flow | |
| Extract unstructured data from medical records and physician notes | Optical character recognition, natural language processing, artificial intelligence | Create a well-structured road map for patients to follow | |
| Case management/ utilization review | Analytics | Lower readmission rate | |
| Population health data management | Analytics | Gain insights for proactive care management | |
| Decision support and treatment options | Artificial intelligence | Increase quality of care | |
| Index-match of CDM with appropriate ICD-10, CPT, HCPCS codes | Analytics | Reimburse accurately | |
| Convert paper EOB to ERA (835) | Automation | Utilize associates for higher value tasks | |
| Identify errors; edit, and resubmit claims | Optical character recognition, artificial intelligence | Reduce administrative burden between payer and provider | |
| Manage claim denials and follow up | Automation; decision support dashboards | Reduce AR days and DNFB KPIs | |
| Manage updates, adjustments, and refunds from the accounting system | Automation and analytics | Improve cash flow |
Source: Infosys, 2019
CDM: charge description master
RPA: robotic process automation
ICD: international classification of disease
CPT: current procedural terminology
HCPCS: health care common procedure coding system
EOB: explanation of benefits
ERA: electronic remittance advice
AR: accounts receivable
DNFB: discharged, not final billed
KPI: key performance indicator
The digital health care gap
The health care industry is behind the curve on digital adoption.
A recent Infosys Digital Radar report reveals that the health care industry scored an average of 41 out of 100 in our Digital Maturity Index.
The low health care industry score compares to an average of over 70 for technology companies and other industries such as financial services, life sciences and utilities, where the average Digital Maturity Index score is around 60 (Figure 3). The legacy incumbents in the health care industry are trying to make progress toward digital transformation, but their efforts are hampered by many complexities and challenges including regulation, security concerns and complex internal processes.
Figure 3. Industry ranking on the Digital Maturity Index
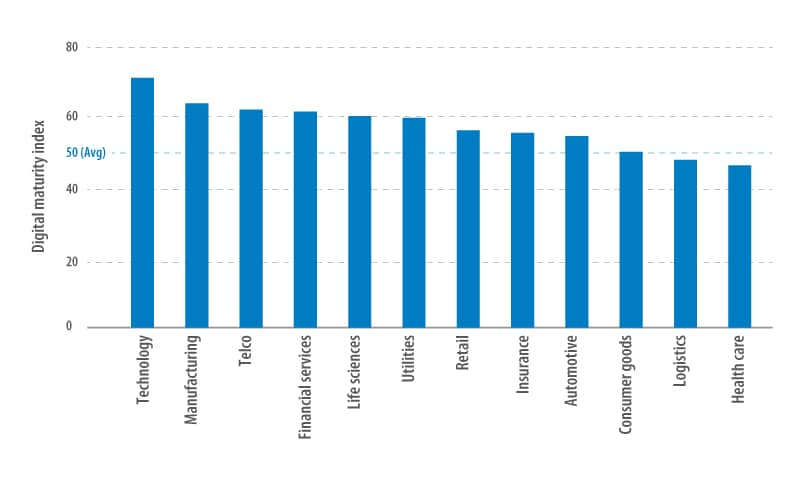
Challenges and complexities
Hospitals across the U.S. have begun to embrace digitization in recent years, not least due to the incentives offered by the government in the wake of the ACA.8 Health care is arguably one of the hardest places to implement digital because of the myriad of challenges and complexities.
Digital transformation for daily operations requires substantial capital investments and cultural change within the organization, with ROI delivered over a couple of years. It’s a big commitment, and leaders cannot be nearsighted in their approach to ROI.
Failure in past digital projects because of inadequate technology, poor integration and lack of change management has made many hospital leaders apprehensive about new projects.
The challenge is multiplied by the numerous and diverse stakeholders typically present within a hospital, including the board of directors, the CEO, the chief information officer, the chief financial officer, physicians, nursing administrators, clinicians, technicians and support staff. Getting everyone together to work toward a common goal is a challenge not to be overlooked.
Hospitals also generate an enormous amount of data in numerous file formats. Data resides in silos, and integration and interoperability are considerable challenges.
Data quality is a problem that stifles digital transformation.
The quality of the data is more important than the quantity when working with sophisticated algorithms.
Related to this are data privacy and security concerns. Hospitals must carefully organize and handle sensitive data. According to the Protenus Breach Barometer,9 the number of patient records breached almost tripled to 15 million in 2018, from about 5.5 million records in 2017, ever increasing the burden of data management and security.
Navigating the way ahead
Health care is high touch, and with the challenges, the stakes are high and complex. The areas of automation have to be selected carefully and providers need to outline and make a targeted set of investments without significant capital outflow in the beginning. It’s essential that hospital leaders consider ROI as well as the value of investment while making investment decisions. In other words, leaders will have to understand the holistic value of investment beyond financial returns.
The patient experience should not be overlooked either. Hospitals with an excellent safety record and patient experience barometer also have better financial performance.
A Harvard Business Review10 study shows that financial margins for hospitals with high customer satisfaction is about 4.8 percentage points higher than the hospitals in the bottom quartile of customer satisfaction.
Embracing the use of cloud-based platforms will also be a big step forward. Cloud-based platforms can help break down data silos and build connected digital experiences. Through migration to the cloud, providers can shift from silo applications to better-integrated and more-modernized enterprise digital platforms that enable digitized operations.
Changes are starting to be made. Forrester11 predicts that hospital CIOs will spend more than their peers in other industries on enterprise health clouds, robotic automation and data security in the coming year. This may be the case, but hospitals still need to have a robust operating framework to ensure that data is stored and used in a trusted and responsible manner. If they don’t start with operational improvements, hospitals’ digital initiatives will struggle to deliver to the top and bottom lines.
References
- https://aharesourcecenter.wordpress.com/2016/05/02/forecasting-hospital-payer-mix-2014-and-2024-u-s/
- https://www.medpagetoday.com/publichealthpolicy/medicare/74009
- http://images.e-navigant.com/Web/NavigantConsultingInc/%7B7900bba7-87bd-4a9b-9cec-54cf0b6ea9d4%7D_HC_HealthSystemFinancialAnalysis_TL_0818_REV08.pdf
- https://www.beckershospitalreview.com/pdfs/Value_of_Time.pdf
- https://www.fiercehealthcare.com/finance/healthcare-supply-chain-association-group-purchasing-organizations
- https://www.modernhealthcare.com/article/20170627/NEWS/170629905/insurance-claim-denials-cost-hospitals-262-billion-annually
- https://healthcare.mckinsey.com/us-healthcare-payments-remedies-ailing-system
- https://www.aimseducation.edu/blog/affordable-care-act-effect-innovations-updates/
- https://www.protenus.com/2019-breach-barometer
- https://hbr.org/2017/05/how-u-s-health-care-got-safer-by-focusing-on-the-patient-experience
- https://www.forrester.com/report/Predictions+2018+Digital+Will+Disrupt+Siloed+Healthcare+Ecosystems/-/E-RES139891







