Optimizing hospital operations through RPA
Robotic process automation has emerged as an effective tool that businesses can use to generate operational efficiencies rapidly. However, it can also be used as the first step on the path toward better data quality that builds a foundation for artificial intelligence and machine learning systems.
It can’t come soon enough for hospitals, which are struggling under the burden of shifting revenue and cost dynamics in an industry that relies on processing large volumes of sensitive personal data. Indeed, at an average of $408 per record, the cost of health care data breaches is at least double that of other industry sectors (see Figure 1). The high cost of a breach is primarily because of the high notification costs and steep penalties in the U.S. for health care information mismanagement. Better management and automation would help significantly reduce the risk.
Figure 1. The health sector faces the highest cost per capita from data breaches
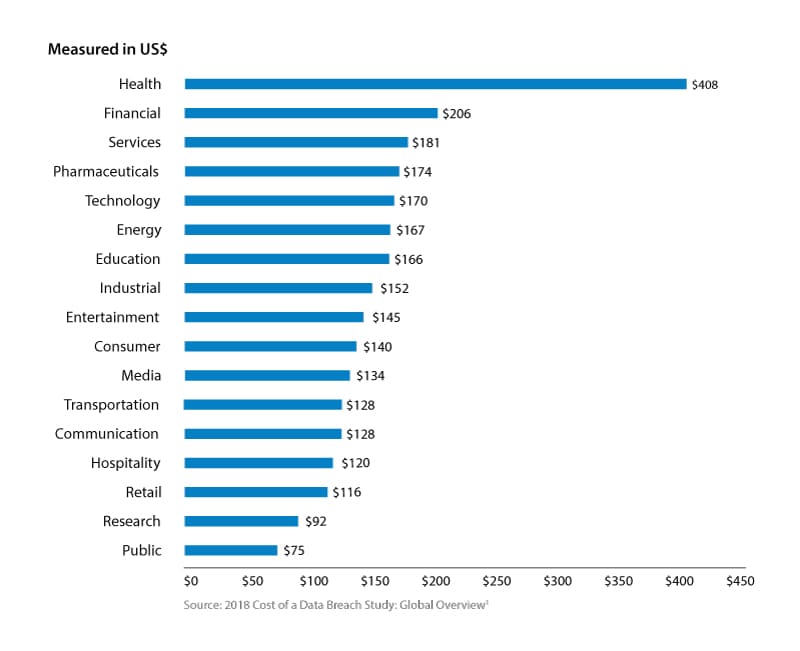
The health sector, in general, is far behind others in adopting digital technologies. According to our recent Digital Radar report, the health care industry scored an average of 41.25 out of 100 in our Digital Maturity Index. This score compares to an average of over 70 for technology companies.
Health care is an industry not considered to be a natural candidate for automation. It is a human-centric service, where the personal touch makes a significant impact on patient experience and outcomes. However, there is still substantial potential for automation given the extent to which data drives decisions and underlying systems. According to McKinsey, 36% of health care activities could be automated, and the majority of the opportunities for automation are around data collection and processing2.
Automation helps reduce today’s data related inefficiencies by improving data quality and consistency, as well as enabling standardized data structures that can create a unified view of performance across a hospital.
Hospitals that have implemented RPA have seen significant benefits. A Kentucky-based multiunit medical services center, upgraded to an integrated medical record and practice management system and saved over 2,000 hours of manual effort. It took the RPA system less than 24 hours to do an error-free transfer of over 64,000 records from legacy systems to a new system3.
In Europe, a general-care hospital with 70,000 emergency visits and 300,000 outpatient visits annually faced several labor-intensive challenges, was dependent on paper records for medical files and financial documents, and had problems managing inventory. The hospital used RPA to eliminate paper records and store data digitally. In the process, it reduced unnecessary functions, integrated operational silos, and streamlined the supply chain. The processing cost of claims and billing decreased from $4 to $1 per claim4.
Where to apply RPA
Robotic process automation is a technology that automates high volume, repeatable business processes by mimicking the human interactions that originally executed the processes.
RPA is best used for mundane and repetitive tasks such as logging into web apps, filling in forms, and pulling data from disparate internal systems (see Figure 2). RPA bots are programmed to follow “if-this-then-that” rules and therefore work well within processes that are already well understood and where the data formats are structured and standardized. However, bots themselves can be used to further structure data through their outputs and can be a vital tool in creating a standardized data architecture.
Figure 2: An overview of RPA, benefits and costs
| What? | How | Benefits | Costs |
|---|---|---|---|
|
|
|
|
In the U.S., missed appointments cost approximately $150 billion annually in physician time and patient health5. RPA can help streamline appointment scheduling and monitor patients after discharge from the hospitals. When patients schedule appointments, the coordinator at the hospital has to align the patient requirements with doctors’ schedules and availability. RPA bots can automate this process; they can collect patient data, such as personal information and insurance details, and schedule appointments according to these criteria. They can even be used to send automated reminders or to update patients when appointments change.
RPA can also be applied to finance functions. Revenue cycle inefficiencies cost hospitals and affect their profits. Claims management is time consuming, and when done manually, it is error-prone. An average 350-bed hospital misses out on $22 million in revenue annually due to inefficiencies in charge capture, account “payables and receivables”, and claims management6. RPA can settle accounts within hours and virtually eliminate human error.
RPA and the road to AI
RPA is foundational for digital transformation. By implementing RPA, hospitals begin a journey of cleansing and standardizing their data and processes in a manner that supports more advanced digital capabilities such as analytics, machine learning, artificial intelligence and cognitive computing. Figure 3 describes the different prospective stages in the digital transformation journey and how RPA fits in the whole scheme of change.
Figure 3. The stages of digital transformation
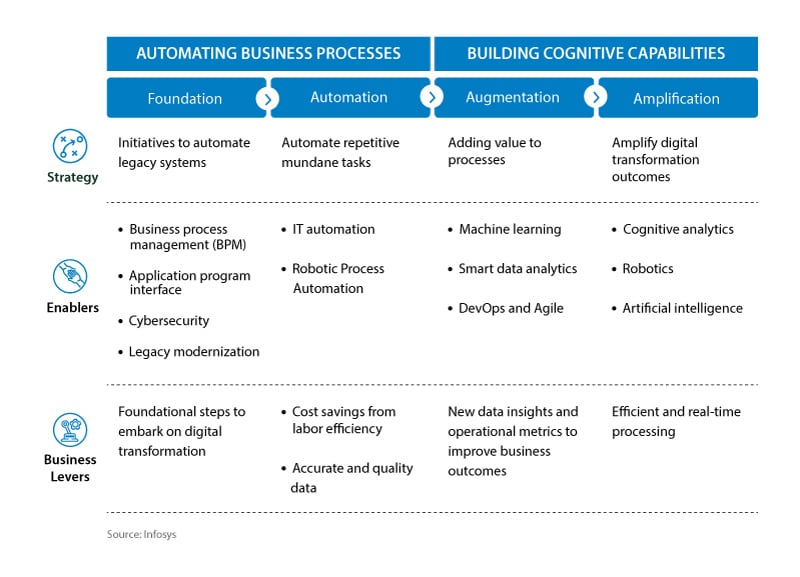
RPA implementation approach
RPA tools can offer significant benefits when deployed correctly. However, poorly planned and executed automation
projects will fail and will risk derailing the broader digital transformation journey.
Given the fundamental shift that RPA enables, an RPA center of excellence should be established to work with each hospital information technology system and its users. The COE should perform the following activities (Figure 4):
Assessment of opportunity:
Identify the processes that are candidates for RPA. The business users of the processes are critical to this activity. Assess whether the given process can be automated using the current RPA platform’s capabilities. Evaluate cost savings and other measurable benefits. Don’t include only waste elimination and error reduction, but also consider the quality of care improvements and health outcomes in calculating ROI. Create a business case for the investment. In calculating ROI, the total cost of automation should include costs of implementation, monitoring performance, production support, and upgrade and change management.
People and process selection:
The core implementation team should be made up of people who understand both the process and technology. The implementation of RPA should also follow the full software life cycle, starting from analysis, bot development, testing and ending with deployment. Change management principles and effective governance of the project plan are critical to the success of RPA implementation. About 30-50% of RPA implementations fail due to poor planning and execution7.
Proof of concept:
Start with a proof of concept followed by a pilot program in noncritical internal processes. Initial successes can help users understand the value of automation. If, for example, hospital leadership and users see a particular process time reduced from 16 to 4 hours, their comfort level will increase and this will generate enthusiasm for broader automation deployment.
Data security:
Throughout the process, data security should be a primary consideration. Single sign-on, username and password conventions, and security matrix optimization should be clearly defined.
Production support:
Support teams monitor automated processes and ensure that the system continues to function per its design.
Scale:
At the design stage of each pilot program, also build a plan to implement the RPA at scale. Without this, an organization can fall victim to “death by pilot,” where new initiatives never scale across the enterprise because stakeholder buy-in, investment planning and change management were not considered at the start.
Figure 4. RPA implementation steps
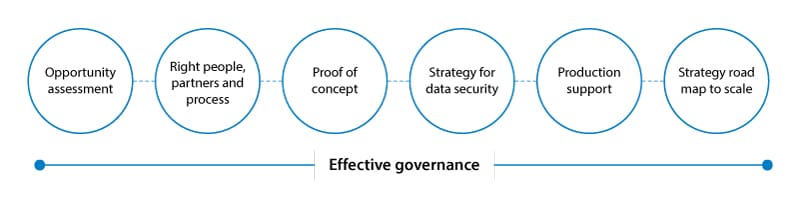
Hospitals and the human touch
RPA is the first small step toward a future where computer systems are more autonomous, and the bigger ambitions of real artificial intelligence can be realized. However, it’s important to keep perspective.
RPA is indeed changing workplace dynamics by taking over activities that humans previously managed. However, for the most part, the aim is not to replace humans. Instead, it can free employees to utilize their potential through more meaningful work that requires social intelligence, complex critical thinking and creative problem-solving.
Nowhere is this truer than in the health care sector, and in hospitals in particular. Care provision is all about the human touch, and the adoption of digital technologies that can increase the ability for medical-care professionals to focus on human interactions must be welcomed.
References
- “2018 Cost of a Data Breach Study,” IBM 2018
- “Where machines could replace humans — and where they can’t (yet),” July 2016
- https://www.automationanywhere.com/solutions/healthcare
- https://www.uipath.com/solutions/industry/healthcare-automation
- “Missed appointments cost the U.S. healthcare system $150B each year,” April 2017
- “You’re probably leaving $22 million on the table,” June 2017,
- https://www.ey.com/Publication/vwLUAssets/Get_ready_for_robots/$FILE/ey-get-ready-for-robots.pdf





